The First 90 Days After Closing on a Dental Practice
Co-Founder, Minty Dental
In Summary
- The first 90 days after closing is when most acquisition problems surface—insurance credentialing delays, staff retention decisions, and cash flow gaps create more pressure than due diligence ever did.
- Insurance credentialing takes 60-90 days on average, meaning you may operate temporarily out-of-network while waiting for approvals—a gap that directly impacts revenue and patient trust.
- Staff retention decisions happen in the first 30 days as your team watches how you handle the first operational crisis, communicate changes, and follow through on transition promises.
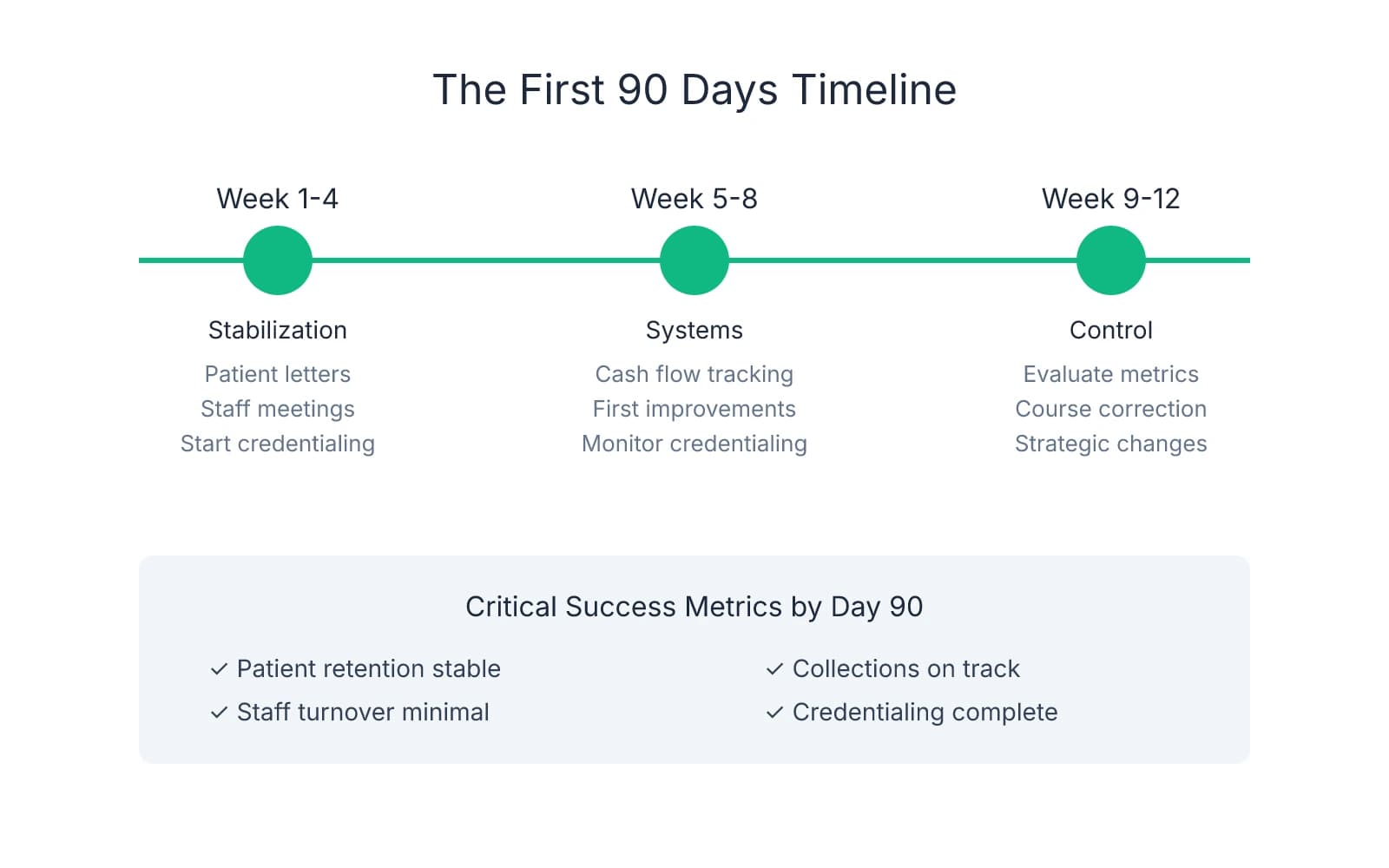
- The transition breaks into three phases: weeks 1-4 focus on stabilization and communication, weeks 5-8 on systems and credentialing progress, and weeks 9-12 on operational control and course correction.
- What you negotiate before closing—seller transition support, staff retention terms, credentialing timelines—determines whether these 90 days feel manageable or chaotic.
The First 90 Days Separate Smooth Transitions from Expensive Scrambles
Closing is when the operational work begins. The first 90 days after taking ownership is when credentialing gaps, staff uncertainty, and cash flow misalignment create the most pressure—and where most acquisition problems surface.
Three predictable challenges define this period. First, insurance credentialing takes 60-90 days on average, leaving you temporarily out-of-network with carriers the practice has participated with for years. Credentialing is tied to the individual dentist at a specific location—even if you're already credentialed elsewhere, you start from scratch at the new address. During this gap, claims may be denied, patients face out-of-network fees, and revenue drops while loan payments stay fixed.
Second, staff retention decisions happen in the first 30 days. Your team is watching how you handle the first operational crisis, whether you follow through on transition promises, and how you communicate changes. Practices that lose key staff in the first month rarely recover the same patient flow or operational rhythm within the first year.
Third, cash flow timing creates pressure most buyers don't anticipate. Collections lag behind production by 30-60 days depending on payer mix, but loan payments, payroll, and supply orders don't wait. If the seller's accounts receivable weren't transferred cleanly or credentialing delays stretch longer than expected, the gap between what you're owed and what you owe widens quickly.
The transition period breaks into three distinct phases. Weeks 1-4 focus on stabilization—communicating with staff and patients, confirming credentialing submissions, and maintaining the seller's systems. Weeks 5-8 shift to systems and credentialing progress—tracking insurance approvals, identifying workflow inefficiencies, and making the first operational adjustments. Weeks 9-12 are about operational control and course correction—evaluating what's working, addressing staff or patient concerns that surfaced, and setting the foundation for the next quarter.
What you negotiate before closing determines whether these 90 days feel manageable or chaotic. Structured seller transition support—ideally 60-90 days with defined responsibilities—gives you someone to answer credentialing questions, introduce you to referring offices, and help navigate the first staff conflict. Staff retention terms reduce turnover risk. Starting credentialing applications 60-90 days before closing can eliminate the out-of-network gap entirely.
The first 90 days is when patients decide whether to stay, staff decide whether to trust you, and insurance companies decide whether your claims get paid. Preparation before closing—not optimism after—determines which side of that line you land on.
Weeks 1-4: Patient Communication, Staff Retention, and Credentialing Setup
The first 30 days set the tone for everything that follows. Three priorities can't wait: communicating the ownership change to patients, stabilizing your staff, and starting the credentialing process immediately.
Send a transition letter co-signed by the seller within the first week that introduces you, reassures patients their care will continue without disruption, and confirms that insurance coverage remains unchanged. The co-signature signals continuity rather than upheaval. During appointments, introduce yourself personally and keep it brief: who you are, why you're excited to serve them, and that their treatment plan stays on track.
Verify that patient communication lists are current and contact information in the practice management system is accurate. If 20% of your transition letters bounce back, you've lost the first opportunity to build trust with a significant portion of the patient base.
Schedule individual meetings with each team member within the first week—not to deliver your vision, but to listen. Ask what's working, what concerns them about the transition, and what they need to do their job well. A hygienist who's been with the practice twenty years knows which patients need extra time—changing the scheduling system in week two without that context creates friction you can't recover from.
Avoid making major changes until you've observed how the practice runs. Staff interpret early changes as a signal that their experience doesn't matter. Committing to a 60-day observation period before implementing new systems doesn't mean you can't address urgent issues—it means you're not redesigning workflows until you understand what problems you're solving.
Start insurance credentialing immediately after closing, but expect 60-90 days before you're fully in-network. Most carriers don't allow you to bill under the seller's provider number unless the seller remains as the treating provider. During the gap, claims may be denied, patients face out-of-network fees, and revenue drops while loan payments stay fixed.
Submit credentialing applications to every carrier the practice participates with on day one. Track each submission separately—some carriers process in 45 days, others take 120. If you're waiting on credentialing to complete before you can bill certain procedures, communicate that timeline to patients upfront.
The seller's transition support is most valuable in weeks 1-4. Negotiate this before closing. Ideally, the seller stays on for 60-90 days with defined responsibilities: introducing you to patients during appointments, answering staff questions about operational quirks, and helping navigate the first insurance or vendor issue. Scheduling a daily 15-minute check-in with the seller during the first two weeks creates a standing window to ask questions as they come up.
Verify that all vendor accounts are transferred to your name and that you have login credentials for practice management systems, scheduling software, and financial accounts. If the supply vendor account is still in the seller's name and an order gets delayed, you're scrambling to reestablish credit terms. If you don't have admin access to the practice management system, you can't pull reports, adjust scheduling templates, or troubleshoot billing issues.
Create a checklist of every system the practice uses—software, vendors, utilities, service contracts—and confirm you have access and ownership transferred within the first week.
Weeks 5-8: Cash Flow Management and Operational Control
Month two is when the financial reality of ownership becomes concrete. Your first month's production won't generate collections for 30-60 days due to insurance reimbursement delays, but payroll, loan payments, and overhead expenses hit immediately. This gap is why working capital—typically 2-3 months of operating expenses—is essential for surviving the transition period.
Practices with strong gross revenue but weak collections often have billing inefficiencies or insurance follow-up gaps that didn't surface until you started reviewing weekly reports. If 30% of your receivables are over 90 days old, you're dealing with a collections problem that predates your ownership.
Pull a profit-and-loss statement, accounts receivable aging report, and production-versus-collections comparison every Friday. If supply costs are running 8% of collections instead of the 5-6% industry benchmark, you need to know in week six, not week twelve.
Rent, lab fees, and payroll are fixed, but supply costs, marketing spend, and equipment maintenance can vary significantly depending on how the practice was managed in the final months before sale. If the seller deferred equipment maintenance or cut back on marketing to improve EBITDA before listing, those costs reappear under your ownership.
You've spent 4-6 weeks observing how the practice runs. Now you're identifying the first operational improvements that won't disrupt patient care: scheduling efficiency, billing follow-up, supply costs. Prioritize high-impact, low-disruption changes first. Tightening your hygiene recall system or implementing same-day billing review doesn't require staff retraining—but both directly improve cash flow within 30 days.
Defer changes that require significant staff adjustment or patient-facing shifts until you have more operational stability. Commit to making no more than two operational changes per month during the first 90 days. This forces you to prioritize what actually matters versus what feels urgent.
If credentialing is still in progress, you're operating partially out-of-network—some patients will face higher out-of-pocket costs. Track credentialing status weekly and communicate proactively with patients whose insurance hasn't processed yet. If 30% of your patient base uses a carrier that hasn't approved you yet, your collections drop while your production stays steady—creating a gap that working capital has to cover.
Staff who seemed supportive in weeks 1-4 may start showing resistance in weeks 5-8 when you begin making operational changes. When you adjust scheduling templates or implement new billing protocols, staff are evaluating whether you're improving the practice or creating more work without understanding their constraints. Frame changes as experiments: "Let's try this for two weeks and evaluate whether it's working." This removes the permanence that triggers defensiveness.
If your front desk coordinator pushes back on a new patient intake process, the question isn't whether they're being difficult—it's whether you've explained the problem you're solving and asked for their input on the solution. Staff retention after acquisition depends less on avoiding all conflict and more on demonstrating that you're listening when conflict surfaces.
Weeks 9-12: Course Correction and Building Momentum
By week nine, you have enough operational data to make informed decisions about what's working and what needs to change. Three metrics tell you whether the transition is on track: patient retention, staff stability, and cash flow trajectory. If any of these metrics are trending negative, months 4-6 are when you address the underlying problems.
Pull a report comparing active patients from 90 days ago to today. If you've lost 10-15% of the active base, that's a signal that patients are choosing to leave rather than stay through the transition. The most common drivers: credentialing delays that forced patients to pay out-of-network fees, staff turnover that disrupted continuity of care, or communication gaps that left patients uncertain about whether their treatment plans would continue.
If patient retention is weaker than expected, the course correction isn't more marketing—it's addressing why patients left. Schedule a review with your front desk team to identify which patients stopped scheduling and whether there's a pattern. The fix might be as simple as a personal outreach call explaining that credentialing is complete and their coverage is now active.
If a key employee announces they're leaving, you're facing a 60-90 day gap to hire and train a replacement. Hiring in a tight labor market takes longer than expected, and new hires need 30-60 days to reach full productivity—meaning the disruption extends well into months 4-6.
Exit interviews matter. If the feedback centers on uncertainty about their role, lack of communication, or changes that felt abrupt, those are fixable problems for the next hire. If the feedback is that they don't trust your leadership, that's a deeper issue that requires addressing your communication and decision-making approach with the remaining team.
Compare your actual collections to your projected collections from the financial model you built during due diligence. If you're running 15-20% below projections, that's not a temporary dip—it's a structural problem. The most common causes: credentialing delays that reduced in-network reimbursements, patient attrition that lowered production, or accounts receivable aging that's worse than disclosed.
Schedule a 90-day check-in with your lender, accountant, and attorney to review financial performance, address any legal or compliance issues, and adjust your operational plan based on actual results versus projections. If your lender sees that you're proactively addressing cash flow gaps, they're more likely to work with you on payment adjustments or additional working capital if needed.
If credentialing is still delayed beyond 90 days, escalate with insurance carriers and consider bringing in a credentialing specialist. If a major carrier—one that represents 20-30% of your patient base—is still pending at day 90, that requires direct escalation to the carrier's provider relations team and potentially hiring a third-party credentialing service.
Implement the first strategic improvements that weren't urgent in weeks 1-8. New patient marketing, hygiene recall systems, treatment plan presentation training, or billing process optimization—focus on high-impact changes that don't require major staff retraining. Tightening your hygiene recare system to reduce no-shows doesn't cost anything, but it can increase production by 10-15% within 60 days.
Avoid launching multiple initiatives simultaneously. One change per month, fully implemented and measured, builds momentum without overwhelming the team.
The first 90 days is not the finish line—it's the foundation for the next 12-24 months of ownership. Months 4-6 are when you solidify the changes made in the first quarter and address any problems that surfaced. If you've identified cash flow gaps, staff retention risks, or patient attrition trends, those require deliberate action and sustained attention.
The transition succeeds when you can answer three questions confidently by day 90: Are patients staying? Is the team stable? Are you collecting what you expected? If the answer to any of these is no, the next 90 days is when you fix it.
Sources & References
The data and claims in this article are drawn from the following sources. We prioritize government data, peer-reviewed research, and established industry publications to ensure accuracy.
- The Hidden Challenge in Dental Practice Transitions — Insurance ...— ameriprac.comIndustry
- How Long Does a Practice Transition Take— ada.orgIndustry
- The Ultimate Guide to Dental Practice Financial Mastery - DSO CFO— dsocfo.com
Navigate Your Practice Transition With Expert Support
The first 90 days set the tone for your success as a practice owner. Minty Plus provides hands-on guidance through this critical transition period, helping you manage operations, staff, and patient relationships with confidence.


